The idea of a universal healthcare system carries many benefits for patients and their families, but in practice, it is not without its risks. The NHS is a prime example of costly issues that can arise when the right infrastructure is not in place. Budgetary constraints have plagued the system for several years, with many calling for a revamp of the organisation to better serve the millions of patients who rely on it each year. Reigning in spending by focusing more on a social care system, adding modern technology tools to create more efficient patient services, and reducing the number of unnecessary procedures and failed treatments is at the core of the NHS plan over the next few years. However, seemingly small issues, including a reduction to ineffective treatment options, have a significant impact on the success – or failure – of the financial revamp of the system.
A recent report highlights this fact, focusing on the added cost of relying on outdated procedures to treat common medical issues. Leg ulcers, which impact an estimated 500,000 adults in the UK, are still being treated through compression bandaging. This traditional method of treatment for leg ulcers is known to be ineffective for many patients, but the recommendation remains the same for hundreds to thousands of patients each year. The NHS faces an additional cost of £2 to £3 million with failed leg ulcer treatments because of compression bandaging recommendations – an expense the system cannot continue to ignore.
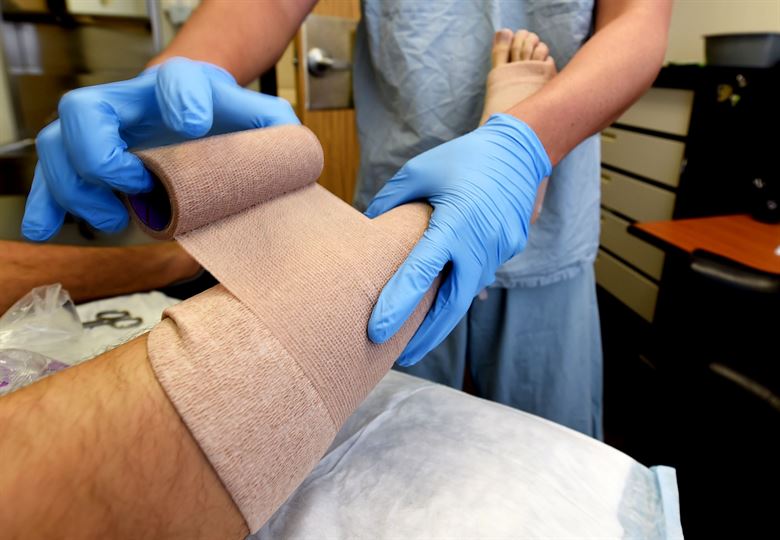
Issues with Compression and Leg Ulcers
Leg ulcers are fairly common among older patients as well as adults with venous disease like varicose veins. When a leg ulcer appears, it is often concerning to the individual because it is an open wound that remains unhealed for several weeks at a time. These wounds cause ongoing pain and discomfort, including itching and swelling. Some of the more severe cases of leg ulcers also result in a foul discharge from the wound and the potential for infection that is not easily remedied after the fact. Most patients are quick to visit their GP for diagnosis and treatment, but when referred to a specialist, only compression bandaging is offered up as a solution.
The issue with compression bandages for use in the treatment of leg ulcers lies heavily on the fact that compression is only a temporary remedy. Placing pressure on the wound with the help of compression bandages allows healthy veins to move the blood throughout the leg. However, compression does little to address the underlying issue that may have caused the leg ulcer in the first place. Despite these realities, NHS providers continually recommend compression bandages when other, more effective treatment options are available.
The Case for Alternative Treatments
According to Dr Eddie Chaloner, a vein specialist at a leading vein clinic in the UK, the use of compression bandages for the treatment of leg ulcers is common in the NHS for several reasons. Many providers are untrained on newer methods of treatment, such as endovenous laser treatment or EVLT. This procedure, which is a minimally-invasive treatment that lasts less than one hour, uses laser technology to dissolve malfunctioning veins in the leg. Once the veins are targeted and destroyed, they are absorbed by the body, allowing healthy veins to resume their job. This type of treatment addresses the underlying cause of leg ulcers for many patients, and it represents a long-term solution instead of a temporary patch.
However, NHS providers are still keen on offering compression bandaging for leg ulcers because it can be an easier, less time-consuming option. Unfortunately, these benefits are short-lived, as many patients return to the NHS after compression fails to fully heal the wound or when the underlying venous disease causing the ulcer creates another issue.
If the NHS wants to truly reign in unnecessary expenses so that it can continue to provide high-quality care to UK patients, focusing on a transition away from short-term, temporary treatments like compression bandaging for leg ulcers is a necessity. Using available resources to train doctors and specialists on updated, more modern approaches to treatment options like EVLT provides a long-term solution. Patients are less likely to return to NHS for follow up visits with additional issues, saving the system money and time.

